Lumbar herniated disc
Last update: 25/09/2018, Dr. Miguel B. Royo Salvador, Medical Board number 10389. Neurosurgeon y Neurologist.
Will my Sciatica get better?
The majority of sciaticas have a cure and in general with an easy treatment.
As for symptoms and the diagnosis
What do I have to do to recover as soon as possible?
95% of sciatica cases heal or improve with rest, lying down and with the help of anti-inflammatories and analgesics.
The body carries out the healing process. The anti-inflammatory improve the inflammation caused by the compression of a nerve root. The analgesics or painkillers alleviate the pain from the nerve root and its territory.
Nevertheless, it is necessary to explain some basic concepts to understanding what happens with a sciatica:
What is sciatic pain or sciatica itself?
It is called sciatica or sciatic pain when the pain coincides with the sciatic nerve path which extends from the lumbar area to the back side of the lower extremity, from which comes lumbosciatic or lumbociatalgia.
If the pain radiates to the front side of the lower extremity, coinciding with the path of the crural nerve, the pain is called cruralgia.
It is important to differentiate between the two as it orients us as to which nerve roots are affected.
What is the cause of sciatic pain?
The sciatic pain, lumbosciatic or lumbociatalgia is frequently caused by the compression of the nerve root by a herniated lumbar disc. But in many occasions, this pain is caused by lumbar facet joints syndrome which is explained further ahead.
What is a herniated disc and a disc protrusion?
A herniated lumbar disc consists of the loss of the cushion situated in the cartilage intervertebral disc that unites two vertebras. The intervertebral disc is formed by a hard external cartilaginous layer called the annulus fibrosa and another that fills the soft center called the nucleus pulpous.
When the annulus fibrosa loses height, tears or breaks and lets out part of the nucleus pulpous, it forms a herniated disc.
As the protrusion or herniated disc occupies an abnormal space, it compresses the structures that are adjacent to the intervertebral disc; if these are the nerves that go to the inferior extremities, it produces injuries which can cause pain, loss of sense of touch and paralysis. Both the protrusion and the herniated disc are considered, for practical purposes, the same but do not indicate in themselves the need for surgery.
There are some wrong concepts, for example, if you have a herniated disc, you must have surgery but not if you have a protrusion. Surgery is not decided by the type of disc alteration but is decided by the clinic and the neurological exploration when dealing with a sciatica caused by disc compression. There are many herniated discs without symptoms and it is not for that reason that they should be operated on. If, on the contrary, there are disc protrusions that produce paralysis, they must be operated on urgently.
What utility does the TC or Scanner and Magnetic Nuclear Resonant (MRI) have?
El TAC y la RM sólo orientan dónde se encuentra y el tipo de compresión nerviosa, en caso de que exista criterio para intervenir nos muestran donde hay que hacerlo. El TAC y la RM no indican si hay que intervenir, ni cuando.
What utility does an Electromiogram (EMG) have in a Lumbociaticaa?
EMG and the electroneurogram (ENG) are a complementary exploration that measure nerve and muscle activity. In a lumbosciatica it advises us as to the type and magnitude of a detectable neurological injury. Not all of the injuries that we see in a neurological exploration are detected in the ENG or EMG.
As for the treatment
How do you cure a lumbosciatica caused by a herniated disc?
Most lumbosciaticas are cured with rest and medical and physical therapy measures which alleviate the consequences of the compressed nerves caused by a protrusion or herniated disc. The organism cures itself when it can restore and consolidate the alteration of the intervertebral disc in a way that there won´t be any active nerve injury or instability or overloaded vertebras.
How do you cure a sciatica caused by a herniated disc?
With an anti-inflammatory treatment we can reduce the inflammation of the nerve compressed by the intervertebral deformed disc and therefore, the pain. With analgesic treatment, the pain is reduced before the anti-inflammatory takes effect, and also while the anti-inflammatory is taking effect, as by itself, it is not enough to alleviate the pain. Rest has two aims, one is to reduce the pressure against the nerve root and to give the organism the possibility to repair the deformity of the intervertebral disc.
How does physical therapy help the lumbosciatica?
Physical therapy has various purposes for a lumbosciatica:
- Mobilize the nerve root so that it accommodates itself and avoids compressing the deformed intervertebral disc and this way alleviates root pressure.
- Relax, stimulate and gratify an area harmed by pain.
- Strengthen the muscles surrounding the vertebras and this way obtain the strengthening of the vertebral.
Physical therapy that applies greater pressure to the intervertebral discs can aggravate the illness and even cause it in other intervertebral discs that are predisposed, that is why physical therapy must be done or directed by an expert of the spinal cord.
What type of herniated lumbar disc is operated?
There are clear criteria for a surgical indication of a herniated disc, it is indicated when the patient present at least two of the following criteria:
- When the lumbosciatic pain is so intense that it does not improve with any medication, or chronic pain becomes so dominant that it prevents a normal routine of life.
- When in the neurologic examination a nervous, motor or sensory affectation is found, especially if it is of progressive character.
- When there are urinary and bowl alterations.
When is a herniated lumbar disc operated on?
When surgery is advised because of acute or chronic pain, it depends on the criteria of the patient and the degree of disability. When surgery is advised because of neurologic impairment, loss of strength, feeling or alterations of the sphincters, the surgery should be done “slowly but surely”. If the loss of strength becomes total, the liberating intervention will not achieve an improvement.
How a herniated lumbar disc is operated?
In the lumbar disc herniation, there are as many diagnoses as clinical histories. Similarly, there are many surgical indications depending upon each patient’s condition as exist as many surgical approaches as surgeons. The end result is the art healing the herniated disc. Generally, there are three purposes in the surgeries lumbar disc herniation: the first and the most important is to release the nerve compression, the second is to fix the vertebral segment and the third is to maintain the height of the intervertebral disc.
By entering this link you can consult the commentary on the protocol followed to choose the type of surgery for the lumbar herniated disc, as performed at the ICSEB. An article called “The lumbar disc herniation in the workplace. Results of a retrospective analysis of a series of 189 consecutive patients.” (Spanish) was published by the Journal of Neurology (Rev Neurol. 1998 Oct; 27(158):574-6). Here the best results of the whole equivalent consulted bibliography mentioned in textbooks and on Medline® database from 1966-1998 were obtained.
Our method in graphic form:
“To look for the best results with the minimum aggression”. The possible techniques that we apply for the surgical treatment of the herniated lumbar disc with contrasting results have the purpose of eliminating the pressure on the nerve root and in some, to preserve the height of the disc and stabilize the spine. They are classified as:
1. Minimally invasive techniques, such as percutaneous nucleotomy and chemonucleoolysis.
2. Microsurgical techniques using protocolized surgical technique to be applied with optical aids.
3. Lumbar laminectomy: an opening in the spine eliminating the posterior portion of a vertebra or lamina of at least one lumbar vertebra.
4. Lumbar arthrodesis: uses fusion systems with or without grafts that solidify vertebras or parts of them.
To choose the most useful technique and at the same time, the least aggressive, it is necessary to clearly specify the type of compression of the nerve root and the condition of the spine.
When we consider that there is only radicular compression, the least aggressive technique is chosen from the first three ones mentioned, according to the size, location and characteristics of the texture of the radicular compression.
If an apparent vertebral instability exists, a lumbar arthrodesis will be indicated. The criterion for instability varies a lot according different surgeons. In our case, we only proceed with lumbar arthrodesis when the lateral functional x-rays, in flexion and extension, show that there is a clear movement abnormality of vertebral column and this can be responsible for the symptoms that the patient suffers. With this criterion only three lumbar arthrodeses were indicated, out of 189 consecutive patients to undergo a lumbar spine procedure; one case with only one bone graft and the others with two instrumented arthrodeses and bone graft. The kind of arthrodesis varies depending on the type of instability and the surgeon’s habits.
Before and after the herniated lumbar disc operation
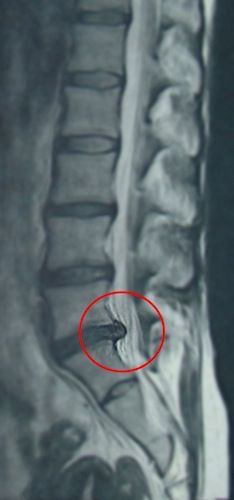
Before the intervención.
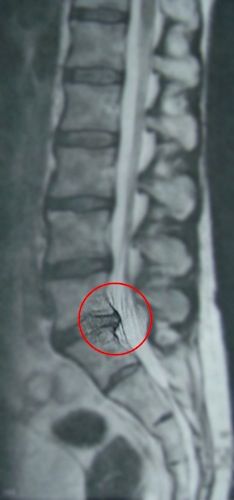
After the intervención.
What is the lumbar facet joints syndrome?
The front part of the vertebrae support each others most important mass or the lumbar vertebrae separated by the intervertebral disc. Behind and on each side they are joined together by the so-called interapophyseal that depend on the height of the intervertebral disc for comfort. If the intervertebral disc decreases in height because the person is standing upright for a long time, the interapophyseal joints become compressed and so cause lumbar pain, or lumbago, in a person without a lumbar disease due to fatigue.
In some patients with interapophyseal joints arthrosis or if the intervertebral disc space, with or without a herniated disc collapses, the interapophyseal joints emit a lumbar pain even at rest. This pain sometimes irradiates downwards towards into the legs without the nerve root being affected to compress the herniated discs.
In cases like these, the patient has the symptoms of a lumbosciatica and nothing appears in the additional testing, the magnetic resonance or CT scans, or on the EMG.
How is the lumbar facet joint syndrome diagnosed (LFJS)?
When a LFJS is suspected, because the patient has lumbosciatica with negative neurological examination and additional testing, the procedure is to give a diagnostic injection with a local anaesthetic when the patient has his/her usual pain. The injection is given into the nerve area of the interapophyseal joint, responsible for the pain, with the help of a x-ray TV machine. If the pain improves, it is a LFJS.
How is SFA cured?
To stop the painful discomfort of SFA , a nerve of the interapofisaria joint is damaged to stop the transmission of pain. This is similar to the way a dentist eliminates the possible pain when a tooth is extracted. There are various techniques, in our case we have selected electrocoagulation with high frequency current for its´ precision and safety, with excellent results.