Last update: 03/20/2026, Dr. Miguel B. Royo Salvador, Medical Board number 10389. Neurosurgeon y Neurologist.
Definition
Odontoid Retroflexion (OR) is a malformation of the upper portion of the cervical spine consisting of a backward tilting of the odontoid process, displacing and compressing the adjacent nerve structures.
It consists of an invagination of the tip of the odontoid process which is abnormally directed backwards, clearly exceeding the imaginary line between the posterior clinoid processes and the postero-inferior angle of the C2 vertebral body.
OR is often associated with Platybasia and Basilar Impression, and sometimes its presence and size does not match the others.
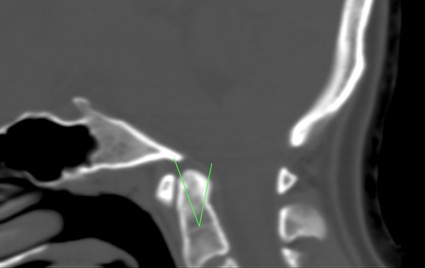
Fig.1 Odontoid Retroflexion. Craniocervical CT.
Symptoms
The symptoms of Odontoid Retroflexion are part of the Basilar Impression and Platybasia picture, the result of compression of the odontoid process on the brain stem and the immediate vascular structures.
The neurological manifestations are typical of a compression of the upper cervical spinal cord: cervical pain, contractures, loss of strength, spasticity, paresis, gait instability, dysmetria and progressive loss of sensation. It may be involved in a chronic increase in intracranial pressure.
Computed Axial Tomography (CT) or Magnetic Resonance Imaging (MRI)
Diagnosis of odontoid retroflexion is radiological, and can be made by CT scan (Fig.1) or MRI (Fig. 2) of the skull or brain and cervical spine or cervical spinal cord.
The diagnosis can be assessed by tracing the Thiébaut-Wackenheim-Vrousos basal line, which is a downward extension of the basal plane, and the odontoid process of the axis is usually tangential, or it is no more than two millimeters away from this line.
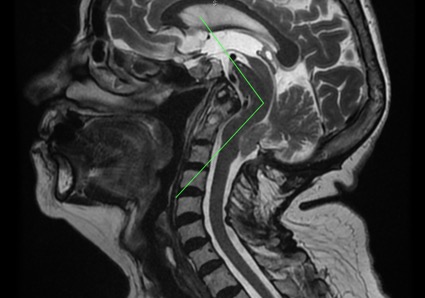
Fig.2.- Sagittal craniocervical MRI showing odontoid retroflexion. Also: basilar impression, descent of the cerebellar tonsils, brainstem kinking. Note the enlargement of the supracerebellar space, evidence for the traction theory and against the theory of the malformation being due to a narrowing of the posterior fossa.
Causes
– According to traditional theories:
Like all anomalies of the cranio-cervical junction, odontoid retroflexion is conventionally attributed to congenital – structural or general/systemic issues – or acquired alterations.
– According to the Filum System ® health method:
The deformity found in odontoid retroflexion is due to a congenital mechanism of asynchrony in growth, in the embryonic phase, between the spinal cord and the central nervous system with the spinal column. This generates an anomalous spinal traction force that is transmitted from the coccyx to the axis (C2) and skull, via the filum terminale. The more intense and earlier this traction is applied, the greater the relevance of the bony manifestations such as odontoid retroflexion.
OR shares the cause of caudal traction produced by an excessively tense filum terminale with the Arnold-Chari Syndrome type I, idiopathic Syringomyelia and idiopathic scoliosis, as well as with other associated malformations of the occipital junction. They are all different manifestations of Filum Disease. The earlier and more intense the onset of caudal traction coinciding with osteogenesis, the greater the bony manifestation such as Odontoid retroflexion, basilar impression and platybasia.
Risk factors
In terms of risk factors, family history plays the most significant role in odontoid retroflexion: it is a congenital condition that can be passed down from one relative to the next. In addition, it shares the same genetic incidence as Filum disease. This pathological mechanism is found in all human embryos, but its clinical translation depends on the intensity, environment, and form of expression of this mechanical conflict.
Complications
In OR, complications may result from the degree of caudal traction or mechanical conflict within the foramen magnum. The latter determines the extent and intensity or degree of conflict between spinal cord traction and brainstem.
- A decrease in Quality of Life can result from torticollis, limited cervical movements, constant cervico-occipital pain, weakness of the limbs, spasticity, gait instability, and loss of sensibility. These conditions can become chronic, progressively increasing and deteriorating the patient’s condition, limiting normal activity.
- In cases of chronic pain, particularly in cases of odontoid retroflexion associated with Arnold-Chiari Syndrome type I or basilar impression, patients may require the assistance of a Pain Management Unit, as first-line anti-inflammatory or analgesic drugs may not be sufficient to alleviate the painful symptoms and headache crises associated with the condition.
- Sudden death may be due to injuries in the cardio-respiratory brainstem nuclei, where the mechanical conflict develops. Respiratory disorders during sleep can be an aspect of the pathology and find expression in the form of apnoeas, respiratory failure, or even sudden death. Hence the importance of early diagnosis and treatment.
Treatment
The conventionally accepted treatment for OR is neurosurgical.
Currently, craniectomy or suboccipital decompression is the standard treatment performed in most centres worldwide for this diagnosis. It is usually indicated mainly in symptomatic cases, as it causes more morbidity and mortality than the natural evolution of the pathology itself.
However, since the publication of Dr. Royo-Salvador’s doctoral thesis in 1993, in which the caudal traction of the entire nervous system by the filum terminale is described as the cause of cerebellar tonsillar ectopia -among other conditions- a new treatment has been developed. This treatment is aetiological, since surgically sectioning the filum terminale eliminates the caudal medullary traction force responsible for the pathological mechanism.
Our technique of sectioning the filum terminale (SFT) is minimally invasive and usually indicated in all cases, symptomatic or not, as soon as possible, since it carries minimal risks, much less than those of the pathology itself, and also stops its progression.
Advantages
1. Eliminates the cause of Odontoid Retroflexion and several associated conditions.
2. Eliminates the mechanism that causes conflict in the craniocervical junction, and with it the risk of sudden death.
3. The mortality rate involved in its application is 0% and there are no sequelae in more than 1500 cases that underwent surgery with the Filum System® method.
4. The surgical time with the minimally invasive technique is of 45 minutes. Few hours of hospitalisation. Local anaesthesia. Short post-operative period without limitations.
5. Improves the symptoms and stops the evolution of the descent of the cerebellar tonsils through the foramen magnum.
6. Prevents hydrocephalus that could ensue because of the impact of the cerebellar tonsils within the foramen magnum, usually associated to odontoid retroflexion.
7. Improves the blood circulation throughout the Nervous System and hence the cognitive faculties that can be affected by the cord traction.
Disadvantages
1. Minimal injury in the sacrum region, with the possible complications of a hematoma or infection of the surgical wound.
2. The improvement of spasticity is sometimes wrongly interpreted as a lessening of strength.
3. The improvement of altered tactile and pain reception sensitivity can wrongly be perceived as an inconvenience.
4. As the blood flow to the brain increases, so does brain activity and mood swings can be observed in the early post-operative period.
Suboccipital Craniectomy:
(Foramen magnum decompression)
Advantages
1. Eliminates the risk of sudden death.
2. Some patients improve clinically.
Disadvantages
1. It does not eliminate the cause.
2. The mortality rate ranges from 0.7 to 12% with a greater surgical risk than the condition’s sudden death rate.
3. Aggressive, mutilating and causes sequelae.
4. It improves the patient’s condition little and for a limited amount of time (estimated in an average of 10 years).
5. Depending on the injury’s location, the surgery itself can cause neurological deficits: hemiparesis (paralysis of a body half) in 0.5 to 2.1%. Visual field alterations 0.2 to 1.4%. Speech alteration: 0.4% to 1%. Sensitivity deficit in 0.3 to 1 %. Instability (difficulty to walk) from 10 to 30%.
6. Post-operative intracerebral haemorrhage, from the surgical site, epidural or intraparenchymal bleeding, that can cause a neurological deficit or increase the pre-existing one, in 0.1 to 5%.
7. Infarction – oedema, variable depending on the process and situation, up to 5%.
8. Superficial deep or cerebral infection from 0.1 to 6.8%, with a formation of a cerebral abscess, aseptic-septic meningitis.
9. Hemodynamic alterations due to the manipulation of the brain stem injuries.
10. Air embolism (patients in seated surgical position).
11. Cerebrospinal fluid fistula or leak 3 to 14% (CSF fistulas)
12. Post-operative hydrocephalus.
13. Pneumocephalus.
14. Tetraparesis (loss of strength in all four extremities) due to the surgical position; incidental.
Sectioning of the Filum terminale: Outcomes
More than 1500 patients have already undergone surgery according to the Filum System® method.
The purpose of the intervention is to eliminate the cause, the mechanical conflict between the deformation and the caudal traction of the entire central nervous system and thus to stop the evolution of the disease, especially the associated neurological manifestations in the case of OR, so that the patient’s quality of life does not deteriorate further.
References
- Dr. Miguel B. Royo Salvador (1996), Siringomielia, escoliosis y malformación de Arnold-Chiari idiopáticas, etiología común (PDF). REV NEUROL (Barc); 24 (132): 937-959.
- Dr. Miguel B. Royo Salvador (1996), Platibasia, impresión basilar, retroceso odontoideo y kinking del tronco cerebral, etiología común con la siringomielia, escoliosis y malformación de Arnold-Chiari idiopáticas (PDF). REV NEUROL (Barc); 24 (134): 1241-1250
- Dr. Miguel B. Royo Salvador (1997), Nuevo tratamiento quirúrgico para la siringomielia, la escoliosis, la malformación de Arnold-Chiari, el kinking del tronco cerebral, el retroceso odontoideo, la impresión basilar y la platibasia idiopáticas (PDF). REV NEUROL; 25 (140): 523-530
- M. B. Royo-Salvador, J. Solé-Llenas, J. M. Doménech, and R. González-Adrio, (2005) “Results of the section of the filum terminale in 20 patients with syringomyelia, scoliosis and Chiari malformation“.(PDF). Acta Neurochir (Wien) 147: 515–523.
- M. B. Royo-Salvador (2014), “Filum System® Bibliography” (PDF).
- M. B. Royo-Salvador (2014), “Filum System® Guía Breve”.
Filum Disease
Dr. Royo-Salvador, with his research and doctoral thesis (1992), proved the theory that considers several diseases of unknown cause (Arnold-Chiari Syndrome Type I, idiopathic Syringomyelia, idiopathic Scoliosis, platybasia, basilar invagination, odontoid retroflexion, brain stem kinking, and others) as part of a new disease concept (the Filum Disease) and that they share a common cause (spinal cord and entire nervous system traction).
The traction force of the entire nervous system in the Filum Disease occurs in all human embryos, hence they all suffer its consequences to a greater or lesser extent, and the consequences manifest in many different ways and intensities.
Other diseases, such as herniated discs, some cerebral vascular insufficiency syndromes, facet joint and Baastrup syndromes, fibromyalgia, chronic fatigue, nocturnal enuresis, urinary incontinence and pronounced paraparesis, are related, due to their cause, to the Filum Disease.
A health method, the Filum System®, has been designed to specify the diagnosis, provide guidance for the treatment and follow-up of: Filum System®.
