1.1 DIAGNOSIS
1.1.1 Can you confirm an Arnold-Chiari Type I / Idiopathic Syringomyelia / Idiopathic Scoliosis diagnosis?
In order to confirm one or several of these diagnoses, you should do and send us the following complementary test results:
MRI of the cranio-cervical region
MRI of the thoracic spine
MRI of the lumbosacral spine
Scoliogram (X-ray of the entire spine on one film, profile and front view)
Once you have the tests and the reports, you can send them through the Internet. We recommend sending your medical files in .zip or .rar format, uploading them to the website https://wetransfer.com/. As an alternative, you can send a copy of your CDs and reports to our postal address in Barcelona. We will provide you with our specialists’ preliminary assessment at distance regarding your case, and we will let you know if they indicate and appointment for a diagnostic conclusion.
1.1.2 I have Arnold-Chiari Type I Syndrome – why do I need MRIs of the thoracic and lumbar spine and a Scoliogram?
Because, according to our studies, this condition tends to be associated to other diseases of the spinal cord and, in order to confirm a diagnosis, our specialists require those test results as well.
1.1.3 What is the meaning of the word “idiopathic”?
From Greek idios (one’s own) and pathos (suffering): “a disease of its own kind, that is not related to any other specific condition”.
The term refers to a primary condition, with no other known cause. Until now, a non-secondary Syringomyelia, i.e. not consequence of a trauma or tumour, was considered to be primary or of unknown cause. The same occurred with Scoliosis, when it was not considered to be traumatic, tumorous, congenital, degenerative, or of neuro-muscular origin.
With his theory, Dr. Royo-Salvador explained the origin of both conditions – an anomalous traction of the filum terminale (a shared etiopathogenic cause).
1.1.4 I have hydrocephalus and Arnold-Chiari Syndrome Type I – can I travel by plane? Can you treat my hydrocephalus?
The possibility to travel by plane with this diagnosis depends on each patient’s clinical condition. We recommend to talk to the general practitioner before taking this decision.
Our neurosurgical service can diagnose and treat hydrocephalus, although we do not provide any exclusive or different solution from other neurosurgical services.
If the patient is not from Barcelona, for the hydrocephalus therapy we recommend contacting a medical centre local to the patient’s place of residence, as the ventriculoperitoneal shunting indicated in this case requires a postoperative follow-up that would not be easily carried out at distance.
1.1.5 What are the “Neuro-Cranio-vertebral Syndrome” and the “Filum Disease”?
The Neuro-Cranio-vertebral Syndrome and the Filum Disease are definitions we use to describe all the clinical expressions related to an anomalous traction of the spinal cord, caused by an overly tense filum terminale. These clinical manifestations may find correspondence with an Arnold-Chiari Syndrome Type I, an idiopathic Syringomyelia, an idiopathic Scoliosis and other conditions.
1.1.6 My Scoliosis curve is more than 40º-50º – will the surgery halt its progression?
In an idiopathic Scoliosis of more than 40º, the curve of the spine depends not only on the traction exerted by a tight Filum terminale, but also on the force of gravity.
With the application of the sectioning of the Filum Terminale, the progression of the curve can be halted, but it can also keep worsening, yet in a slower manner than it would without treatment.
In these cases, our medical team will provide the most adequate postoperative indications for each patient: rehabilitation, physical therapy and/or brace.
1.1.7 As my Scoliosis curve is more than 50º, orthopaedists and traumatologists indicated a spine fixation. Why and when (before or after) would I have to undergo the sectioning of the Filum Terminale (SFT)?
Our medical team treats idiopathic Scoliosis according to a neurological and neurosurgical perspective. In idiopathic Scoliosis, the tension that occurs within the spinal canal affects the spinal cord. With the application of the SFT it is possible to eliminate the tension and the force exerted by the Filum Terminale, which generates the curves.
This surgery is fundamental. If possible, it is recommended to apply the SFT before the spinal fusion, in order to avoid the risk of paraplegia that the latter entails, since the traction of the spinal cord increases as it is straightened.
Even if the patient has already undergone the fusion procedure, it is convenient to apply the SFT. In fact, this will reduce the traction of the spinal cord caused by a tense filum terminale, which adds to the tension of straightening the vertebral canal.
1.1.8 If I have Scoliosis, why do I need to have a magnetic resonance done?
Our Institut is a neurosurgical centre; it studies and treats Scoliosis in the perspective of the spinal cord within the scoliotic spine. The MRIs are necessary to examine the state of the spinal cord within the vertebrae. The Scoliogram (full spine x-ray), on the other hand, allows examining the bony part of the vertebral column only.
1.1.9 Are these diagnoses rare in children?
Like in adults, the diagnosis of Filum Disease with Arnold-Chiari Syndrome Type I, idiopathic Syringomyelia and/or idiopathic Scoliosis is not rare in children, in fact it affects far more patients than believed in the past. The diagnosis in children is actually far more difficult than in adults: on one hand, they are still not able to properly describe their symptoms and, on the other, diagnostic MRI is applied exclusively when there is a strong suspicion or given incidental findings related to other conditions and tests, as sedation is required. Hence, the incidence can be even higher than the actual detection rate. At our centre, we have seen and diagnosed more than 250 children (boys and girls) between 0 and 10 years of age and over 70 cases between 0 and 5 years of age with the previously mentioned pathological combinations.
1.1.10 Can the diagnosis of disc herniations and protrusions be related to the Filum Disease?
The increase in intradiscal pressure, due to the cord traction, may cause the rupture of the annulus fibrosus with minimum physical strains and weights. That is why disc protrusions and herniations are more frequent when associated to the Filum Disease or the Neuro-Cranio-vertebral Syndrome according to the Filum System® diagnosis.
1.2 INDICATION OF SURGICAL TREATMENT
1.2.1 What should I do when a specialist indicates the application of a surgical treatment?
The indication for a surgical treatment must be considered after an extensive review of the case and of all factors, such as possible diagnoses and treatments, the patient’s age, quality of life, expectations, etc.
1.2.2 When is the application of the Filum System® surgical protocol recommended in the Filum Disease?
Once the condition is diagnosed, the application of the surgical treatment is recommended as soon as possible, in order to eliminate the cause and halt the progression of the disease. A diagnosis of Filum Disease implies the existence of a progressive physical deterioration, especially neurological.
1.2.3 Are there cases of asymptomatic patients with an anatomical expression of the condition (through MRIs and X-rays)?
In over 3000 first medical consultations at our centre, we have not had a single case of an asymptomatic patient. In the clinical examination or in the medical history, we have always identified signs or symptoms of the disease, of which neither the patient nor their health professionals were aware. In our clinical experience we found different types of circumstances in patients with Filum Disease:
- Patients with many symptoms and/or signs and little anatomical expression of the disease:
Without a specialist review of MRIs and X-rays, many patients with these characteristics do not find a diagnosis (example: very slight descent of the cerebellar tonsils; image of ischemia-oedema in the spinal cord, as expression of a Pre-Syringomyelia; deviation of the vertebral column of less than 10º in Scoliosis). This usually delays the diagnosis and the treatment, thus risking a further worsening of the patient’s neurological condition.
- Patients with few symptoms/signs and a significant anatomical expression of the disease:
Some patients find out by chance that they have the disease, through an MRI. If they believe they have no symptoms and their quality of life is acceptable (as they do not know it without the disease), they decide not to undergo surgery. In this type of cases, it is also recommended to apply the Filum System® as soon as possible, as there is always a physical deterioration. Furthermore, some symptoms (frequently the loss of strength and of sensitivity in the head and extremities) or lesions that go unnoticed, might aggravate until reaching an irreversible stage. The descent of the cerebellar tonsils or the intramedullary cyst can also involve a risk of brainstem compression within the foramen magnum. This, together with the traction force that generates tension and impaction, could not only compromise the quality of life, but even put life itself in danger (risk of sudden death).
- Patients with symptoms/signs and no anatomical expression:
The Filum Disease has been diagnosed in some patients who could not find an anatomical cause for their clinical pictures compatible with the disease (examples: impaction of the cerebellar tonsils, Arnold-Chiari Syndrome Type 0, clinical Neuro-Cranio-vertebral Syndrome). After an extensive examination of the brain, brain stem and spinal cord and having previously excluded other comorbidities, our specialists indicate the application of the Filum System® with excellent results.
- Patients with severe anatomical expression and apparently no symptoms:
Many neurosurgeons, who do not agree with the Filum System®, suggest waiting for symptoms to appear before operating, sometimes even in cases with a significant descent of the cerebellar tonsils or large syringomyelic cavities. That is because their treatment of choice is Decompression, sub-occipital craniectomy, which has a higher risk than the most severe anatomical expressions of the condition itself and can cause a far worse clinical picture for the patient. On the other hand, the neurosurgeons that apply the Filum System® recommend the surgery even with apparently no symptoms: in fact, this method proved that there are no asymptomatic cases, at least as far as signs, reflexes and alterations are concerned. The condition is already active, therefore they recommend operating as soon as possible, to prevent existing injuries with apparently no symptoms from getting worse and avoid additional anatomical deteriorations, which affect the patient’s clinical condition.
1.2.4 Why are some neurosurgeons advising to wait before applying a surgical treatment?
When the treatment of choice for Arnold-Chiari Syndrome Type I is decompression or sub-occipital craniectomy and for Idiopathic Syringomyelia it is Syringostomy, they recommend observation instead of surgery, in some cases. These are major surgical interventions, with higher risks and more frequent complications than those of the condition itself. Therefore, if the condition does not yet compromise the patient’s quality of life significantly and the symptoms are not that serious, the specialists who apply these techniques consider that it is not necessary to operate.
1.2.5 Are there cases where it is recommended to wait before applying the Filum System®?
The Filum System® surgical protocol for the sectioning of the filum terminale, to be applied in the Filum Disease, in general involves minimal risk. There is only a remote possibility of infection or hematoma of the wound, as with any other surgical procedure. Therefore, it is recommended to apply it as soon as possible, once the condition is diagnosed; the purpose is to eliminate the appearance of tissue lesions, as occurs in all cases diagnosed with the existence condition, with a minimal surgical risk, almost null compared to that of the condition itself.
1.2.6 How do the Filum System®, decompression and syringostomy surgeries affect the Filum Disease?
The Filum System® eliminates the root cause of the disease – not its consequences – with the objective of halting its progression. In many cases, although the action is not addressed to the disease’s effects, there can be an ascent of the cerebellar tonsils, a reduction of the syringomyelic cavity, or a straightening of the curved spine. An early intervention can prevent symptoms from worsening and help improve those that are reversible at the moment of the surgery.
On the other hand, sub-occipital decompression and syringostomy do not eliminate the root cause of the disease (“Syringomyelia, scoliosis and idiopathic Arnold-Chiari malformations: a common etiology”, Rev Neurol. 1996 Aug; Volume 24, Nº 132; 937 – 959, Royo-Salvador) – the anomalous traction produced by an overly tense filum terminale – so the disease remains active. This explains why symptoms often reappear years after the sub-occipital decompression (“Hindbrain decompression for Chiari – syringomyelia complex: an outcome analysis comparing surgical techniques”, C. Hayhurst, O. Richards, H. Zaki, G. Findlay & T. J. D. Pigott, Department of Neurosurgery, Walton Centre for Neurology and Neurosurgery, Liverpool, UK).
1.2.7 I have Arnold-Chiari Syndrome Type I with/without Syringomyelia: your specialists indicate the Sectioning of the Filum Terminale, while another neurosurgeon recommends a Craniectomy. Do you have cases of a Craniectomy applied after the Sectioning of the Filum Terminale?
In over 1500 cases operated by means of the sectioning of the filum terminale according to the Filum System® method, we never have considered it necessary to re-operate by applying a suboccipital craniectomy. We know that a few of our patients, after the sectioning of the filum terminale, consulted other specialists for a second opinion and underwent a sub-occipital craniectomy, searching an improvement of irreversible sequelae or lesions that could have gotten better in the long term. On the other hand, we applied the Filum System® sectioning of the filum terminale in several patients that had previously undergone one or more decompressions, and obtained significant improvements.
1.2.8 What does the post-operative course depend on?
It depends on how early the Filum System® is applied, starting from the surgical protocol, following with rehabilitation and check-up consultations in the years after the surgery. We know that, if on one hand the majority of patients report several improvements, on the other, the post-operative course depends on the actual reversibility of the injuries at the moment of the sectioning of the filum terminale. That is why we recommend its application before irreversible lesions occur due to the anomalous traction of an overly tense Filum terminale.
1.2.9 Which surgery is applied for disc herniations and protrusions, according to the Filum System® method?
In general, in patients with Filum Disease and associated disc disease, we observed that a positive post-operative course is possible after the surgical release of the cord traction, with improvements both at a clinical level and in the neuroimaging.
In those cases with severe disc disease, persistent or worsening symptoms, we recommend the surgical removal of the herniated disc in the same operative session or after. The most frequently applied technique in lumbar herniated discs is the discectomy via semi-hemi-laminectomy, while for thoracic disc herniations it is the transartrectomy; in the case of cervical disc herniations, a discectomy via anterior approach with the placement of a graft or intersomatic cage is applied.
1.3 SURGICAL PROCEDURE
1.3.1 How is the Sectioning of the Filum Terminale surgery performed with your technique?
With the minimally invasive Filum System® SFT technique, the ligament is sectioned in the sacral region, without touching the bone or having to open the medullary membranes. The size of the surgical wound is of few centimetres and has no external stitches. In adults, local anaesthesia with sedation is applied, unless there are contraindications.
1.3.2 Where is the scar going to be located? Will it be very visible?
It will be on the coccyx, in the sacral region, at the end of the spine and at the beginning of the intergluteal cleft. It will hardly be visible or, with time, not even be noticeable.
1.3.3 What risks and complications can this surgery involve?
The only risks or complications of the SFT as performed by our medical team can be a hematoma or an infection of the surgical wound, if the post-operative guidelines are not followed. These include amongst others: avoid physical strain that affects the surgery area and do not wet the wound during ten days after surgery.
Like any surgical procedure, also the SFT can be subject to circumstances that are external to the surgical technique itself, like those related to anaesthesia or other external factors.
1.3.4 After sectioning the filum terminale, will my spinal cord be moving around inside?
The sectioning of the filum terminale eliminates the anomalous traction force that is applied on the patient’s spinal cord and nervous system. With the surgery, the nervous system is released, but there is no change in tissues position.
Only in some cases we detect that the conus medullaris and the descended cerebellar tonsils, over time and very slowly (usually years after the surgery), may ascend by some millimetres.
1.3.5 Does the filum terminale have a function? Is anything going to happen if it is sectioned?
The filum terminale ligament has a function during the embryonic development, but not after. Hence its sectioning in childhood, adolescence or adult age does not have any negative consequence.
1.3.6 Does the patient’s age affect the Sectioning of the Filum Terminale treatment according to your Filum System®?
Age does not influence the disease, as its evolution occurs in a unique and individual way in each patient. In a sample of more than 800 cases, we have observed infant patients with a very affected spinal cord, as well as others in adult age that were not that much affected, and vice versa. What has been detected as influential in the outcomes of the surgery is the evolution of the injuries of the nervous system, not the patients’ developmental age.
Given this general characteristic of randomness in the expression of the Filum Disease (with Arnold-Chiari Syndrome type I, Idiopathic Syringomyelia, Idiopathic Scoliosis), once the indication of surgical treatment has been confirmed, it is recommended to undergo the procedure as soon as possible, in order to stop the evolution of the lesions.
1.3.7 At what age do you start to operate? Did you perform the Sectioning of the Filum Terminale in children?
We know by experience that the Sectioning of the filum terminale should be applied as soon as possible in order to stop the evolution of the disease. Therefore, it is convenient to schedule the surgery as soon as the cord traction condition is detected, without any contraindications from early childhood.
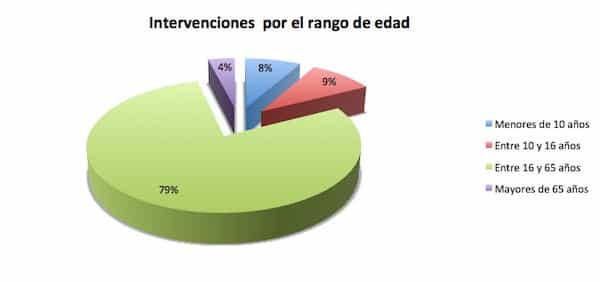
Out of the total population of operated cases at our Institut by means of the Sectioning of the Filum terminale with the minimally invasive technique at our Institut – with diagnoses and combination of diagnoses included in the Filum Disease – 8% are children aged 0 to 10 years. Currently, the youngest patient who underwent surgery with our team was 4 months old at the moment of the treatment.
In children, general anaesthesia is usually administered; however, this is ultimately determined based on the anaesthesiologist’s criteria.
1.3.8 Did teenagers undergo surgery with your technique?
Out of the total population of operated cases at our Institut by means of the Sectioning of the Filum terminale with the minimally invasive technique at our Institut, 9% are children and teenagers aged 10 to 16 years. With them, general anaesthesia is usually administered. Conventionally in medicine, patients older than 16 years are considered as part of the adult age group of patients and if there are no contraindications, local anaesthesia with sedation is administered. However, this is ultimately determined based on the anaesthesiologist’s criteria and protocols.
1.3.9 Did elderly patients undergo the Sectioning of the Filum Terminale? Up to what age do you apply this treatment?
Out of the total population of operated cases at our Institut by means of the Sectioning of the Filum terminale with the minimally invasive technique at our Institut, 4% of patients are older than 65 years.
According to our centre’s philosophy, we help patients by applying surgical treatments, provided that the surgery’s benefits can improve the patients’ quality of life, even if only for a few years.
The most senior patient who underwent the SFT surgery with our team was 86 years old at the moment of the procedure.
1.3.10 Can it be an inconvenience if the surgery date coincides within the menstrual period?
No, the patients’ stage in the menstrual cycle does not involve any inconvenience.
1.3.11 Can the filum get tethered again?
After the SFT, there exists a possibility of “retethering”, or adhesion, of the sectioned extremity of the filum terminale to the surrounding structures. It has been documented with extensive bibliography that with the intradural SFT there is a retethering rate between 1% and 55%, depending on the author (Stone and Rozzelle 2010, Cochrane et al 1998).
For the SFT technique as applied by our team, with the sectioning of the filum terminale at its coccyx insertion, there is no existing bibliography. In our experience of more than 1500 operated cases, we are aware of one case of clinical retethering, that is to say with the re-appearance of the symptoms or signs of the disease due to which the patient underwent surgery in the first place.
1.3.12 Why does the ® symbol appear next to the Filum System® method’s name?
The highly specialised clinical experience of our surgical team lead our centre to the development of etiopathogenic, diagnostic, medical, surgical and rehabilitation treatment protocols, that came to define the Filum System® health method. The method was registered as a trademark in 2013, as a guarantee of quality for excellent medical and surgical practice.
The Institut Chiari & Siringomielia & Escoliosis de Barcelona is a highly specialized centre that holds the Management System certification according to the UNE-EN ISO 9001:2008 standard. The ICSEB is the only centre in the world legally authorized for the application of the Filum System® surgery.
1.3.13 There is a doctor in my country that says that he/she is performing the same surgery as Dr. Royo – can I trust him/her?
The Filum System® is our Institute’s unique and exclusive method and at the moment there are no other centres or neurosurgeons in the world accredited for its application. Unless a doctor appears in our list of Filum System® Surgical accredited centres or specialists, beware of anyone who claims he/she applies the same method.
1.4 OUTCOMES
1.4.1 In Arnold-Chiari Syndrome type I, can the descended cerebellar tonsils ascend after the SFT?
In the majority of cases operated at our centre, the descent of the tonsils at the level of the foramen magnum and/or the brain stem does not vary upon sectioning the filum. What disappear immediately with surgery, are the pressure on the nervous tissue within the foramen magnum caused by the cord traction and the risk of cardiorespiratory dysfunctions involved in the affected area where the cardiorespiratory nervous centres are located.
However, we observed in some cases, 2/3 years after the surgery, an ascend of the cerebellar tonsils by a few millimetres; sometimes they even reposition themselves completely.
1.4.2 Will the symptoms disappear after sectioning the filum?
The application of the Sectioning of the Filum Terminale aims to stop the evolution of the disease. The injuries that the nervous system has suffered as a consequence of the disease may be reversible or irreversible. The symptoms associated with reversible lesions, connected to tissues that are not functioning but that are not dead either, may see recovery. The symptoms due to dead tissue, in case of being nervous tissue, do not disappear. This is why the release of the spinal cord should not be delayed, once the cause of the anomalous traction is detected.
1.4.3 I underwent a suboccipital craniectomy surgery (with classical or minimally invasive technique) – will this affect my post-Sectioning of the filum terminale outcome?
In Arnold-Chiari Syndrome type I patients, who have already undergone one or more sub-occipital craniectomy, depending on the post-operative reversible or irreversible sequelae and on possible associated conditions, the outcomes of the Sectioning of the Filum Terminale could be partial if compared to those of patients who have opted for the application of the Filum System® method only.
At the ICSEB we do not assess the technique of choice for the sub-occipital craniectomy – be it classical or minimally invasive –, as this surgical treatment is dismissed as an option according to the theory at the base of Dr. Royo-Salvador’s studies of more than forty years.
1.4.4 Are the syringomyelic cavities going to disappear after the SFT?
Syringomyelia consists of cysts that develop within the spinal cord as a result of the lack of blood flow caused by the Filum Disease. Once the traction exerted by an overly tense Filum Terminale is eliminated, with the application of the FS® method, the existing cavities stop increasing further and the ischemia-oedema does not progress. Subsequently, we can observe a development of the cysts, which over time tend to collapse and disappear in most patients, as Dr. M. B. Royo-Salvador described in his Doctoral Thesis (“Aportación a la etiología de la Siringomielia”, 22 Dec 1992, Universidad Autònoma de Barcelona).
1.4.5 Is the progression of scoliosis going to stop after the SFT?
Our medical-surgical team, in their experience with more than 620 operated patients (until November 2016) with Idiopathic Scoliosis – associated or not with other diagnoses –observed that the development of scoliosis of less than 40º stopped with the application of the Filum System®.
1.4.6 In the case of scoliosis, is it possible that the spine will straighten up after the sectioning of the filum terminale?
For some patients with scoliosis of less than 30º it is possible to experience a reduction in the curvature. Depending on the case, this may happen spontaneously or require the help of physical therapy or wearing braces.
1.5 POST-OPERATIVE PERIOD
1.5.1 After the surgery, what do I have to prepare for (recovery, medication, rehabilitation, follow ups)?
After the Sectioning of the Filum Terminale with minimally invasive technique, the main recommendation is not to wet, contaminate nor wash the surgical wound for 10 days. After that time period, and with a physician’s clearance, showers are allowed, however full baths are not permitted until 40 days after surgery.
Starting from the first days after discharge, depending on each patient’s pain sensitivity in the surgical area, it is possible to return to a normal life, go to work and/or school, provided that these activities do not involve physical strains, such as lifting weight or maintaining static or repetitive positions that can compromise the wound.
About 40 days after the operation, a post-surgical check-up is recommended, during which, based on the state of the wound healing, the doctors will allow to return to a completely normal activity and provide instructions for rehabilitation, physical therapy and sports activities depending on the individual case.
The next check-up is scheduled one year after surgery, with the preoperative and new neuroimaging exams, to compare the evolution of the injuries observed before surgery.
1.5.2 I am not from Barcelona and I have already returned home after the SFT. If I notice blood or pus in the surgical wound, can you help me? Who should I contact?
We recommend that recently operated patients, who are no longer in Barcelona and experience issues with their surgical wound or clinical state, immediately approach an emergency service, their family doctor or a trusted surgeon. We invite them to keep us informed so that our neurosurgeons can provide advice and care guidelines.
1.5.3 If I undergo surgery, how long will it take before I can return to my usual activities?
It takes at least 40 days for the surgical wound to scar correctly after the SFT. For the first 10 days it is recommended not to wet the wound. Afterwards, with a doctor’s clearance, showering is allowed but not taking a bath until day 40.
We recommend returning to usual daily activities whilst avoiding physical strain. It is permitted to go to work or to school once back home, as long as these activities do not involve lifting weight or other physical efforts that could affect the wound area.
In the 6-weeks check-up, rehabilitation indications will be provided if necessary, or the return to the most appropriate sports activity will be discussed.
1.5.4 I experienced a significant improvement after the SFT, but now I feel I am getting worse again. What is happening?
In the post-operative period of the Sectioning of the Filum terminale, there can be fluctuations of symptoms and clinical manifestations with decrease and/or increase in intensity/frequency/duration. These ups and downs may occur episodically during the first month, or possibly during several months after the surgery.
We observed that the majority of patients find a new stability in their symptomatological picture one year after the surgery; for others this occurs from the first postoperative day, and others experience it later on, after one and a half or two years.
It is important to remember that the clinical evolution and its long term phases must be monitored together with the specialist, who will provide an objective assessment of the changes.
1.5.5 After the SFT, the doctor recommended physical therapy. For how long should I do it?
The instructions and duration of post-surgical rehabilitation are different for each patient, depending on many factors, such as the degree of involvement, the reversibility (or not) of the injuries, the possibility to access physical therapy centres, the healthcare conditions and possibilities in the patient’s home territory.
Our specialists will prescribe physical therapy during the check-up appointment one month after the SFT.
1.5.6 I have been to physiotherapy centres and they said that, since I underwent surgery abroad, they will not take charge of my case. What can I do?
Our Institut collaborates directly and reciprocally with internationally accredited FS® rehabilitation centres and professionals, who follow the exclusive Mantia-Royo Protocol of physical therapy.
If your home physiotherapy centre cannot assist you in planning a postoperative treatment, you can consult our partners who will provide you with personalized guidelines to bring home with you. If this option is not possible for personal reasons, our surgical team can prepare a referral for a rehabilitation treatment.
1.5.7 What will the post-SFT long-term clinical evolution be like?
After the surgery, patients may experience some fluctuations of the pre-existing symptoms. Their condition will tend to find a new balance in a few weeks, months, or in approximately one year.
We have observed that the nervous system is able to restore reversible injuries and functions that have been compromised by the disease over a period of many years, up to 10 or 15 years.
1.6 ICSEB’S METHOD AND OTHER CENTRES’ METHOD
1.6.1 How is the sectioning of the filum terminale performed at the Institut Chiari & Siringomielia & Escoliosis de Barcelona?
The Filum System® standard surgical technique for the Filum Disease is exclusive and original of our Institute and is based on almost 50 years of experience of its creator, Dr. Miguel B. Royo-Salvador.
It is a minimally invasive procedure, anatomically adapted to each clinical case, in order to be the least aggressive as possible. We observed no major complications, except hematoma or surgical wound infection in exceptional cases. The traditional method for the sectioning of the filum terminale by means of lumbar laminectomy – with a duration of approximately 4 hours under general anaesthesia – has been reduced to a 40-minute intervention under local anaesthesia and outpatient setting (with only one night of hospitalization in observation, for the patient’s comfort).
1.6.2 Does the Filum System® method always apply the same procedure of the sectioning of the filum terminale? Or does it include other possibilities?
Depending on the different pathological expressions of the Filum Disease and the associated diagnoses, the Filum System® can provide for both the standard sectioning of the filum terminale and variations applied to each specific case. Furthermore, additional techniques can be applied in the same surgical session. For example, in the case of severe herniated discs, it is recommended to operate them together with the SFT, to ensure excellent results. Therefore, the neurosurgical indication is confirmed only after a full diagnostic consultation.
1.6.3 What is the difference between your technique for the sectioning of the filum terminale and those offered by other surgeons in my country?
We currently know that no other centres apply the sectioning of the filum terminale for the treatment of Arnold-Chiari Syndrome type I, idiopathic Syringomyelia and idiopathic Scoliosis. They do apply it only for the diagnosis of Occult tethered cord syndrome. The difference between our and other centres, therefore, not only lies in the surgical method (which in the case of the Filum System® is unique, original and of highest standard), but also in the time, place and way of operating.
1.6.4 Why should I choose the Institut Chiari de Barcelona to undergo surgery?
Understanding the cause of a disease is extremely important in medicine, as it allows to indicate the most appropriate treatment for each patient and to obtain the best possible results.
The team of specialists at our centre follows Dr. Royo-Salvador’s innovative theory, according to which Arnold-Chiari Syndrome type I, Idiopathic Syringomyelia and Idiopathic Scoliosis share the same root cause: the abnormal spinal cord traction which is exerted by the filum terminale. Also other conditions are considered to be a consequence of this traction and the Filum System® method can identify them. Our specialists consider that by sectioning this ligament, the tension that generates these conditions can be released and, by treating also the other associated ones – such as herniated discs or spinal stenosis – the lost quality of life can be restored as far as possible.
Hence, follow-up consultations, personalized postoperative care and rehabilitation instructions according to the Filum System® protocols are extremely important in order to obtain excellent surgical results for these diagnoses.
1.6.5 Why shouldn’t I consult other surgeons who perform the sectioning of the filum terminale in my country?
As far as we know, other surgeons are applying the sectioning of the filum terminale, but exclusively as a treatment for the Occult tethered cord syndrome (diagnosis for which this intervention had been conventionally conceived) and not for other conditions, such as those associated with the Filum Disease. Therefore, we fear that the application of the sectioning of the ligament in Filum Disease cases with Arnold-Chiari Syndrome type I, Idiopathic Syringomyelia and Idiopathic Scoliosis, not only might be based on a technique that is not as refined as ours, but could also be inadequate in both its indication and follow-up. All this is due to the lack of knowledge regarding the Filum Disease and of the evolution that it can produce in these diagnoses.